Core Services
Dry Eyes
What are Dry Eyes?
Exactly as it sounds, dry eyes result when tears can’t provide enough lubrication for the eyes or if the eye is producing poor quality tears. In a healthy eye, tears are spread across the cornea and help provide clear vision with every blink. Their purpose is to keep the eye surface smooth and clear, provide lubrication, wash away foreign matter, and help reduce the risk of eye infection.

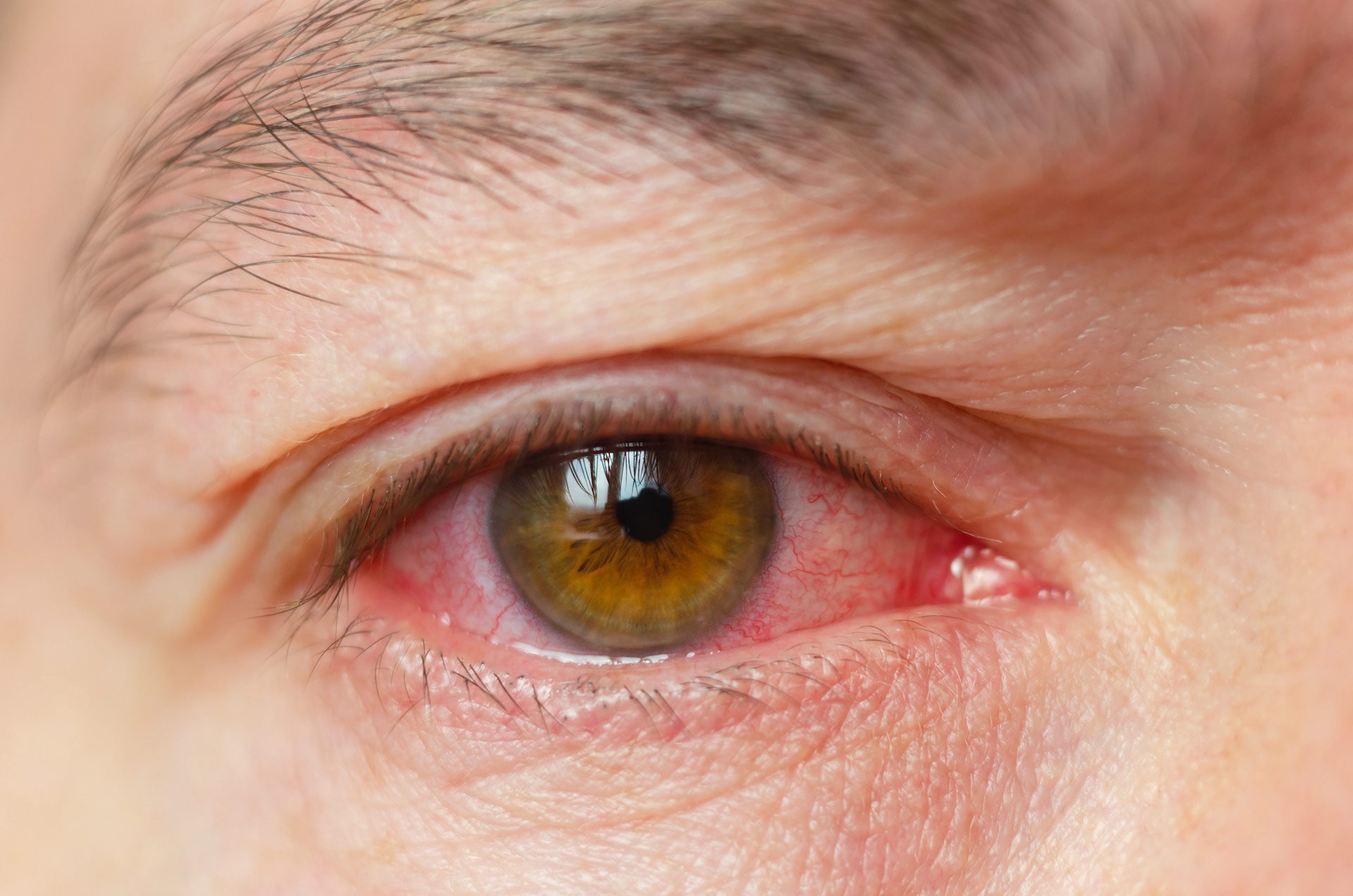
Symptoms
When dry eyes occur, grittiness, stinging, and/or a feeling general uncomfortableness can be experienced, leading to inflammation and damage of the eye’s surface. Other symptoms include:
- Redness
- Scratchiness or burning sensations
- Sensitivity to light
- Watery eyes
- Stringy mucus in or around eyes
- Blurred vision
- Difficulty driving in the dark
- Feeling that something is in eyes
- Difficulty wearing contact lenses
Risk Factors
Dry eyes can develop for many reasons, but some people are at higher risk:
- Age 65+
- Females – due to hormonal changes caused by pregnancy, oral contraceptives, and menopause
- Medical conditions – rheumatoid arthritis, diabetes, thyroid problems, inflammation of the eye surfaces or eyelids
- Medications – antihistamines, decongestants, blood pressure medications, and antidepressants can reduce tear production
- Situational circumstances – exposure to windy situations, on an airplane, after a long duration of screen time
- Long-term use of contact lenses

Dry Eyes Treatments
There are several options available to treat dry eyes including:
- Eye Drops / Oral Medications
- Punctal Plugs
- LipiFlow
Eye Drops / Oral Medications
Over-the counter eye drops, called artificial tears, are one of the most common ways to treat dry eyes, especially for minor to moderate symptoms. These work by simply moistening the eye, however, they may need to be used several times per day. Avoid using eye drops that reduce redness; these can cause more irritation as they constrict blood vessels.
Alternatively, ointment can be applied, but it does tend to cloud vision, so it is recommended that it is used only before bedtime.
For more chronic cases of dry eyes, antibiotics or anti–inflammatories may be prescribed in the form of oral medication or eye drops to reduce inflammation of the eyelids and stimulate oil production in the oil glands around the eyes.
Your ophthalmologist will provide suggestions for the best drops/ointments to use.
Punctal Plugs
Puncta is the formal name for the small openings in the tear ducts that drain tears from the eyes. By inserting a tiny plug into the tear duct, this opening in the inner corner of the upper and lower eyelids is closed, allowing the eye to conserve both naturally produced and/or any artificial tears. By retaining fluid, the eye’s surface remains moist; hence alleviating dry eyes and the effects associated with them.
Two Types of Punctal Plugs
Temporary Plugs
These are often used after having refractive surgery, such as LASIK or SMILE to keep the eye moist, or for trial purposes so a patient can if they help with their particular dry eye situation. Made from collagen, the plugs gradually break down and dissolve, lasting for a period of a few days to months.
Semi-Permanent Plugs
Designed to remain in the eye for a longer period (i.e., years), these plugs are made from a more durable medical material like silicone or acrylic and require an ophthalmologist to remove. There are different options for this type of plug – those inserted closer to the surface and those placed in a deeper part of the tear duct called the caliculus, which cannot be seen at all in the eye.
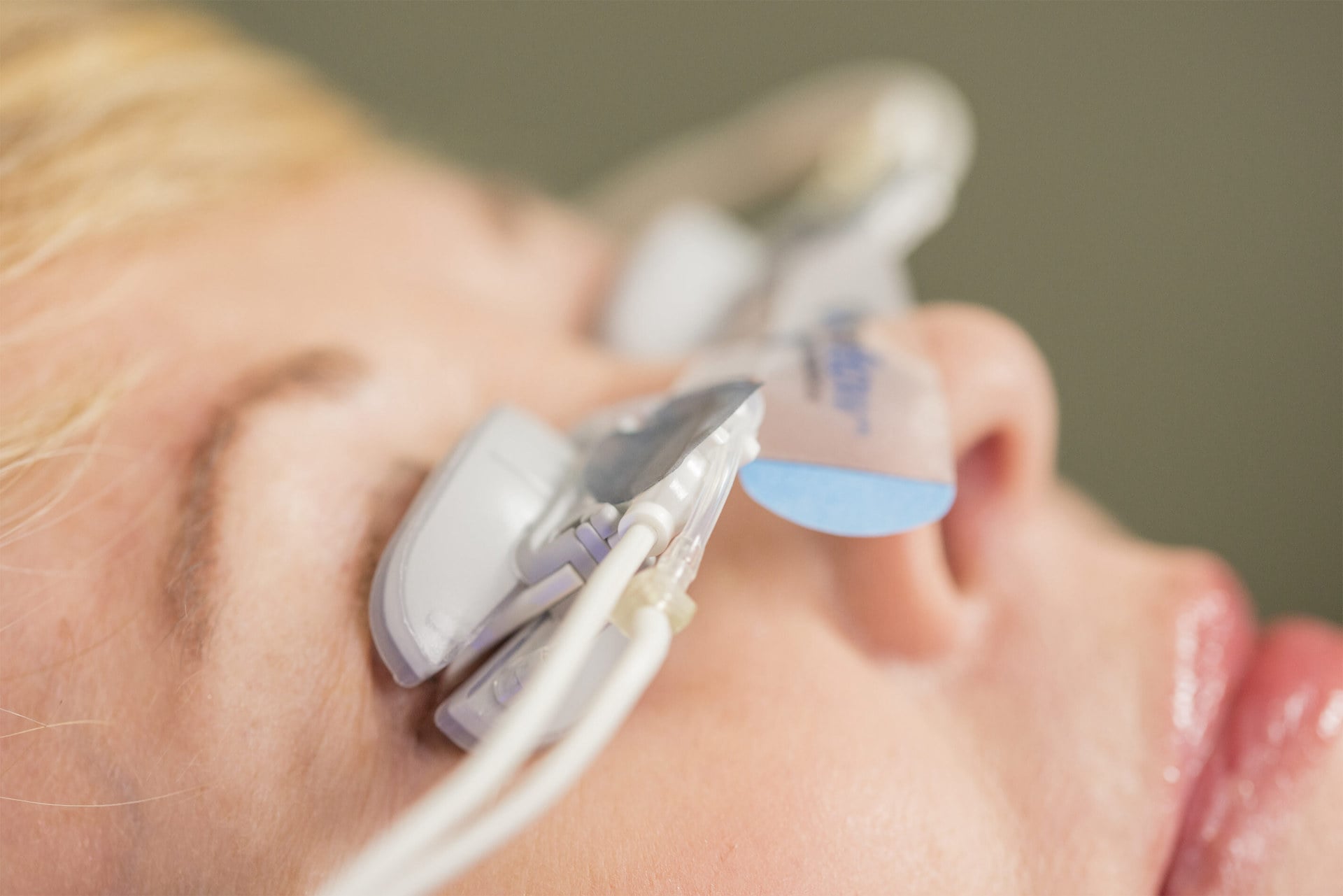
LipiFlow
If eyes don’t respond to traditional treatment, LipiFlow Thermal Pulsation System could be a viable solution. This non-invasive treatment utilizes the latest technology with heat and massage to clear obstructed glands in the upper and lower eye lids. This procedure unblocks the meibomian glands for those that suffer from meibomian gland dysfunction (MGD) due to:
- Effects of certain medication
- Pregnancy or post-pregnancy
- Contact lens wear
- Autoimmune diseases such as lupus or rheumatoid arthritis
Once determined that you are a candidate for LipiFlow, the non-invasive procedure takes only 12 minutes in total with a three-step process.
LipiFlow Procedure
- Step 1: Numbing drops will be inserted into the eyes to ease any potential discomfort.
- Step 2: The LipiFlow system’s activators—dome-shaped, single-use sterile devices—are placed on your eyes.
- Step 3: Using Vector Thermal Pulsation technology, the activators send heat into the glands inside your lids and massage out any blockages.
LipiFlow is not covered by OHIP, but the procedure is offered through Clarity Eye's Comprehensive Dry Eye Care Program (CODEC).